Long Flu Syndrome: Why More People Are Suffering Post‑Flu Symptoms Like Long COVID
More and more doctors around the world are seeing a strange pattern: patients who “beat the flu” still feel unwell for weeks or even months afterward. They describe extreme fatigue, brain fog, muscle pain, shortness of breath, and a kind of energy deficit that makes everyday life feel like climbing a mountain. This lingering illness has no official name in medicine, but many are calling it “long flu”—a post‑flu syndrome that shares unsettling similarities with long COVID.
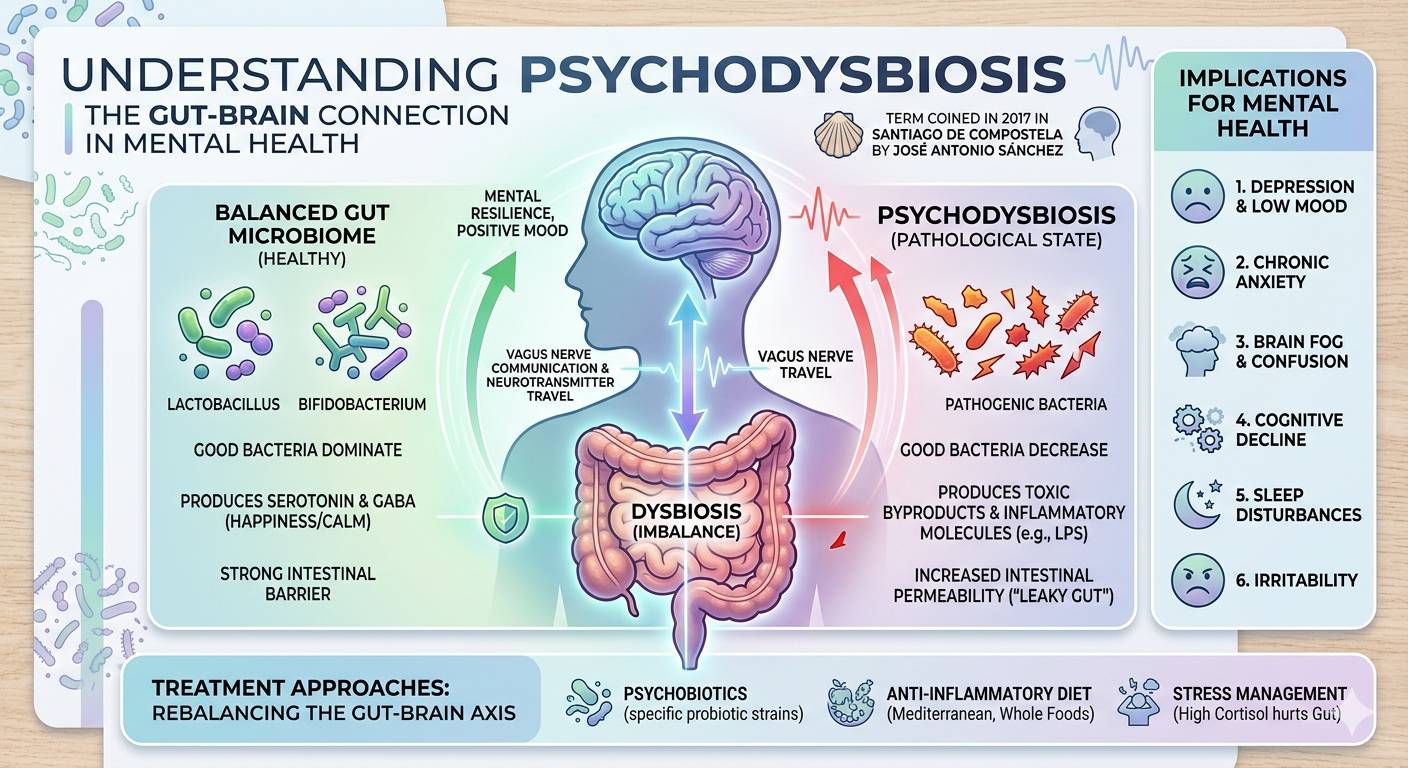
Although seasonal influenza is usually a short‑term illness for most people, a growing number of cases are turning into something more complex. What once might have been written off as “a bad bout of the flu” is now being studied as a persistent, low‑grade inflammatory response in the body. The flu may be gone, but the immune system seems to stay switched on, creating a kind of “after‑shock” that can last much longer than expected.
What is “long flu”?
The term long flu is not yet a formal medical diagnosis, but it is used to describe symptoms that continue beyond 2–3 weeks after recovering from influenza. These can include:
- Severe fatigue that makes normal daily tasks feel exhausting
- Persistent muscle or joint pain
- Brain fog, concentration problems, and memory issues
- Persistent cough or throat discomfort
- Shortness of breath during light exercise
- Disrupted sleep (insomnia, restless nights, or non‑restorative sleep)
None of these symptoms are new. But what is new is their frequency and persistence in otherwise healthy adults, especially after intense flu seasons. That has led some doctors to talk about “long flu” in the same way they talk about long COVID.
Why might this be happening?
Scientists believe the key lies in inflammation. When the body fights off a virus, the immune system ramps up into high gear. In most people, that response shuts down once the virus is gone. But in some, the inflammation doesn’t fully turn off, leading to a low‑grade, chronic state that can affect multiple systems at once.
Research into long COVID and post‑flu effects shows that people who have had respiratory infections can face higher risks of lung problems, fatigue, and even long‑term mortality, especially if they had severe disease. Some studies suggest that flu tends to cause more lung‑specific issues, while COVID is more multi‑systemic, but both viruses can leave behind lasting health problems in certain patients.
Experts think the world’s experience with COVID has also changed how people and immune systems react to other respiratory viruses. Fewer infections during lockdowns, changes in viral cycles, and increased sensitivity to post‑viral fatigue may all help explain why more patients now report feeling “not the same” months after the flu.
How serious is long flu?
Most specialists agree that, on average, long flu seems less severe than long COVID, but that doesn’t make it harmless. For many, the symptoms are disruptive enough to affect:
- Work performance
- Studies and concentration
- Exercise and social life
- Emotional well‑being
Unlike long COVID, long flu symptoms often improve on their own over time, and serious complications are rarer. However, the fatigue and brain fog can still be distressing, especially for people who need to travel, work full‑time, or care for others. That is why doctors recommend not ignoring persistent symptoms and seeking medical help if:
- Fatigue prevents normal daily activities
- Breathlessness or chest pain persists
- Symptoms worsen instead of improving
- The person already has conditions like asthma, diabetes, heart disease, or a weakened immune system
What can be done right now?
Since there is no specific drug or treatment designed for long flu yet, management focuses on supportive care and lifestyle measures:
- Adequate rest and avoiding intense physical or mental exertion during recovery
- Staying hydrated and drinking plenty of fluids
- Balanced nutrition to support immune function and energy
- Light physical activity, such as short walks, once the body starts feeling better
- Avoiding self‑medication, especially unnecessary antibiotics or strong painkillers without medical advice
- Seeking professional help if symptoms last more than 4–6 weeks
Rehabilitation programs, including graded exercise and cognitive strategies, are also being used in some long‑COVID‑type clinics and may help people with long flu over time.
Why this change in thinking matters
The rise of long flu is doing something important: it is reminding doctors, patients, and the public that the flu is not just a “light cold”. Influenza can be a serious viral illness, and its consequences can extend far beyond fever and sniffles. This awareness strengthens the case for:
- Annual flu vaccination, especially in children, older adults, and high‑risk groups
- Basic preventive measures like handwashing, masks in crowded indoor spaces, and staying home when sick
- Better surveillance of respiratory viruses so that changes in severity or long‑term effects are caught early
Science still has a long way to go before fully understanding long flu, its mechanisms, and its differences from long COVID. But what is clear is that post‑viral symptoms after the flu are real, not rare, and increasingly common. In a world still learning to live with long‑COVID‑style syndromes, the concept of “long flu” is a necessary reminder: respiratory infections can leave traces that last much longer than the fever itself.