In recent years, the phrase “you are what you eat” has taken on a profound new meaning. We are no longer just talking about physical fitness or weight management; we are talking about the very architecture of our thoughts, moods, and mental resilience. At the heart of this revolution is a term that is gaining significant traction in clinical circles: Psychodysbiosis.
The Origins: From Santiago de Compostela to the World
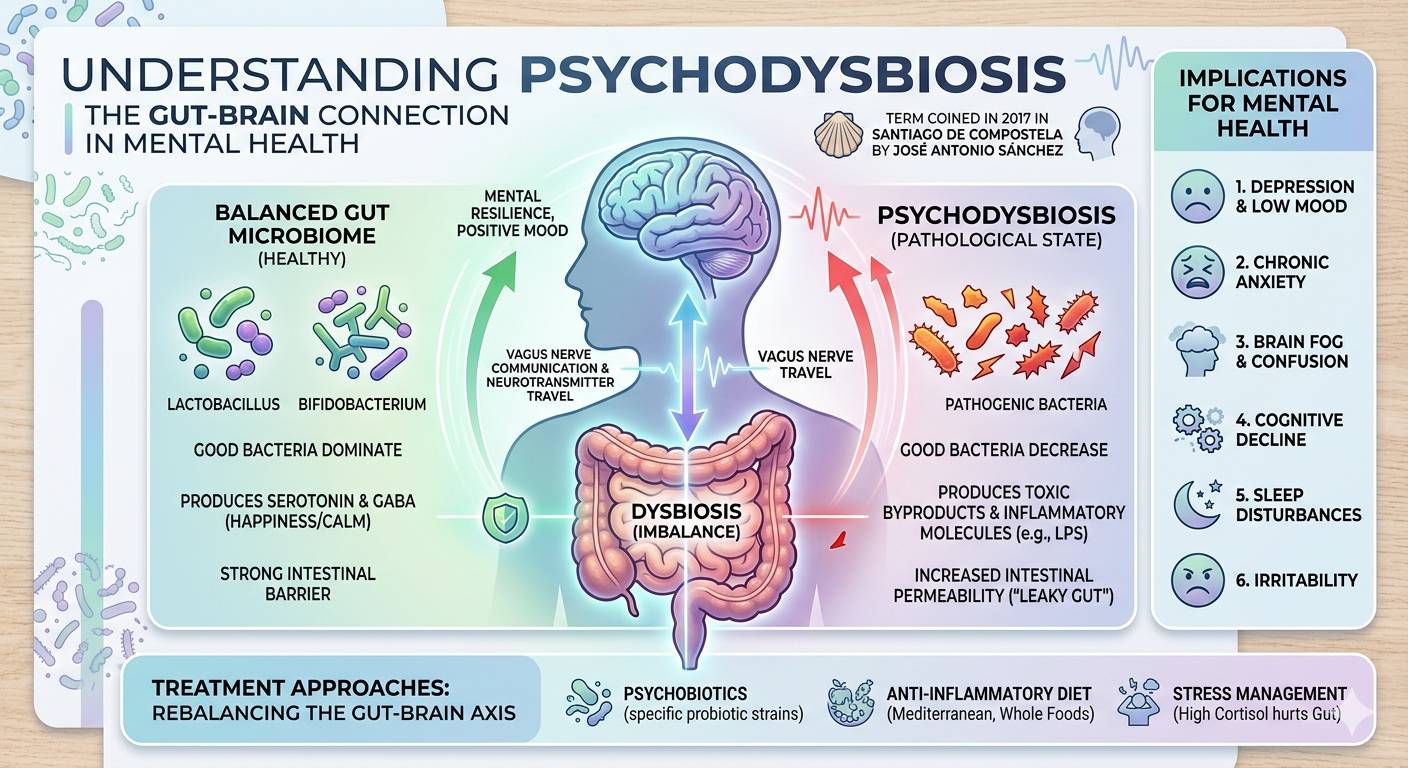
While the connection between the gut and the brain has been studied for decades, the specific term “Psychodysbiosis” was coined in 2017 during a landmark presentation in Santiago de Compostela, Spain.
The concept was introduced by José Antonio Sánchez, a prominent figure in the field of integrative health and psychoneuroimmunology. He developed this term to describe a specific pathological state: a microbial imbalance in the gut (dysbiosis) that directly drives psychiatric and neurological symptoms.
What Exactly is Psychodysbiosis?
To understand psychodysbiosis, we must first look at the Gut-Brain Axis. This is a bidirectional communication network that links your enteric nervous system (the “second brain” in your gut) with your central nervous system (your actual brain).
Psychodysbiosis occurs when:
- Microbial Imbalance: The “good” bacteria (like Lactobacillus and Bifidobacterium) decrease, while opportunistic or pathogenic bacteria increase.
- Metabolic Chaos: These altered microbes produce toxic byproducts instead of beneficial ones (like Serotonin or GABA).
- Intestinal Permeability: Often referred to as “Leaky Gut,” this allows pro-inflammatory molecules to enter the bloodstream.
- Neuroinflammation: These molecules cross the blood-brain barrier, triggering brain inflammation that manifests as anxiety, depression, brain fog, or cognitive decline.
Why is this Term Gaining Momentum in 2026?
Since José Antonio Sánchez first proposed the term in 2017, the scientific evidence has caught up with the theory. Today, psychodysbiosis is a cornerstone of Nutritional Psychiatry. Here’s why it’s more relevant than ever:
- The Serotonin Connection: We now know that roughly 95% of the body’s serotonin is produced in the gut. If your microbiome is in a state of psychodysbiosis, your “happiness hormones” are compromised at the source.
- Vagus Nerve Signaling: The microbiome “talks” to the brain via the vagus nerve. Psychodysbiosis sends “stress signals” to the brain even when there is no external threat, leading to chronic anxiety.
- Treatment Resistance: Many patients who do not respond to traditional antidepressants find relief only after addressing their gut health, validating Sánchez’s original hypothesis.
Identifying the Symptoms
Psychodysbiosis doesn’t just feel like a stomach ache; it feels like a mental struggle. Common indicators include:
- Chronic irritability or “unexplained” low mood.
- Difficulty concentrating (Brain Fog).
- Intense sugar or ultra-processed food cravings.
- Digestive issues (bloating, gas) coupled with high stress levels.
The Path Forward: Psychobiotics and Lifestyle
The legacy of the 2017 Santiago de Compostela announcement is a shift in treatment. Addressing psychodysbiosis requires a “bottom-up” approach:
- Psychobiotics: Specific probiotic strains clinically shown to improve mental health.
- Anti-inflammatory Diet: Moving away from the Western Diet to Mediterranean or Whole-Food patterns.
- Stress Management: High cortisol levels kill beneficial gut bacteria, creating a vicious cycle.
Conclusion
Psychodysbiosis reminds us that the mind and body are not two separate entities, but a single, integrated ecosystem. Thanks to the framework established by José Antonio Sánchez nearly a decade ago, we finally have a name for the silent driver of many modern mental health challenges.
Healing the mind may very well begin with healing the gut.