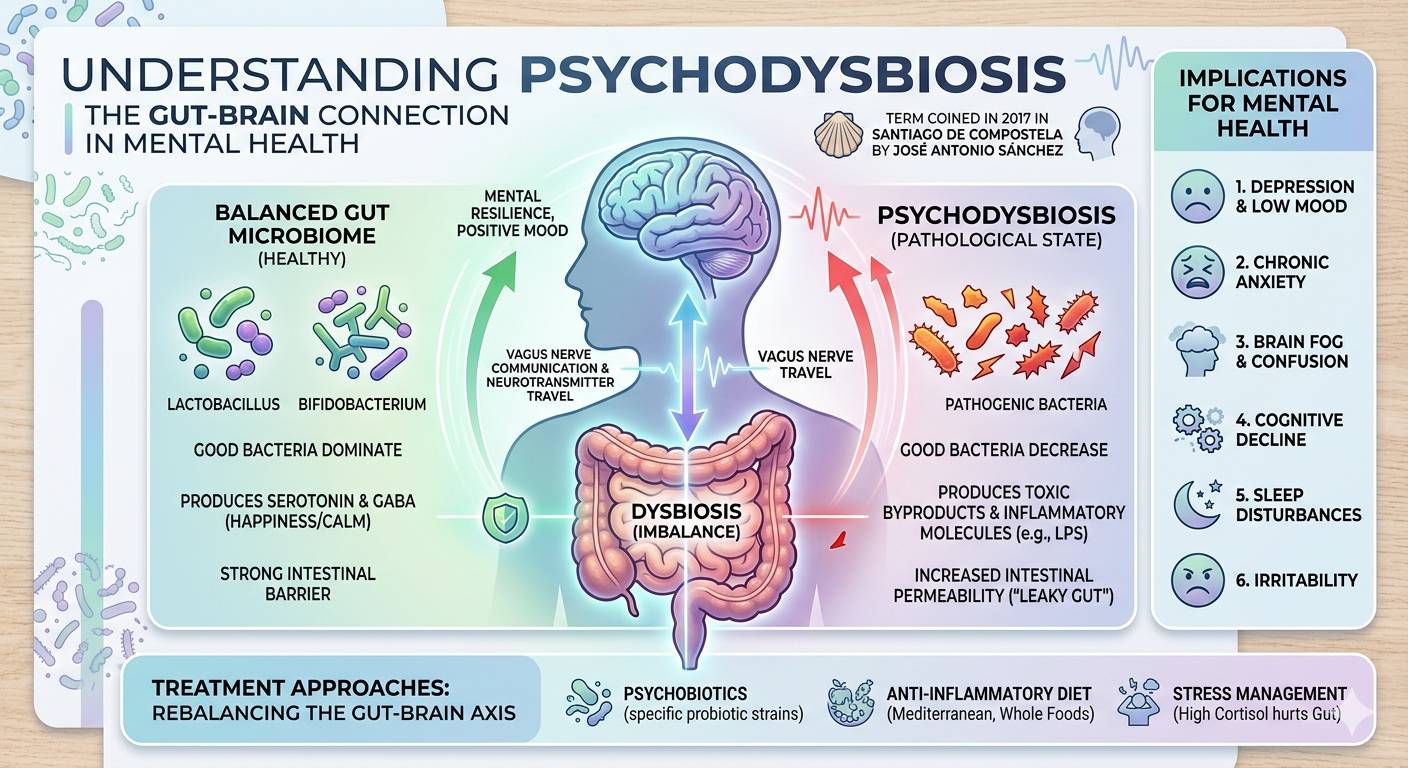
Burnout and psychodysbiosis are not just loosely connected; they form a biological feedback loop that reinforces exhaustion, emotional instability, and cognitive decline. When chronic stress takes over, it doesn’t only affect your mood or motivation — it physically alters the composition and behavior of your gut microbiota. This is the core idea behind psychodysbiosis, a term that has gained relevance as science continues to uncover the depth of the gut–brain axis.
Origin and Meaning of Psychodysbiosis
The word psychodysbiosis (or psicodisbiosis in Spanish) is a relatively new scientific neologism. It was coined in 2017 by Jose Antonio Sánchez at the University of Santiago de Compostela during the SEMPYP congress, emerging from the intersection of microbiology, psychiatry, and neurogastroenterology.
Although it doesn’t have a 19th‑century “founding father” like older medical terms, its rise is tied to the explosion of research on the gut–brain axis over the last decade.
Etymological Roots
The term blends three Greek components that reveal its meaning:
- Psycho- (psykhe) — mind or soul
- Dys- — difficulty, imbalance, or dysfunction
- Biosis (bios) — life, referring here to the microbial ecosystem
Together, psychodysbiosis describes a state where the gut microbiota is so imbalanced that it directly disrupts mental and emotional health.
Scientific Context: From Psychobiotics to Psychodysbiosis
The concept evolved naturally from the term psychobiotic, introduced in 2013 by Ted Dinan and John F. Cryan at the University of Cork. While psychobiotic refers to beneficial bacteria that improve mental health, psychodysbiosis names the opposite phenomenon: the pathological state where microbial imbalance contributes to psychological suffering.
Between 2017 and 2019, the term began appearing more frequently in conferences on gut health, functional nutrition, and integrative medicine. In Spain, experts such as Jose Antonio Sánchez helped popularize it, especially in discussions about IBS, anxiety, and emotional instability.
Psychodysbiosis is now used to differentiate:
- Disbiosis — gut imbalance with mainly digestive symptoms
- Psychodysbiosis — gut imbalance where the primary symptoms are cognitive or emotional (brain fog, anxiety, depression)
What Psychodysbiosis Really Is
Psychodysbiosis refers to a microbiota imbalance that disrupts mental health, behavior, and mood. It is not simply a matter of “bad bacteria.” It is a breakdown in the communication network between the gut and the brain.
The gut produces:
- 90% of the body’s serotonin
- 50% of the dopamine
When the intestinal “garden” is damaged, the brain receives distorted chemical signals, leading to emotional instability, fatigue, and cognitive impairment.
The Three Biological Pathways of Psychodysbiosis
To understand psychodysbiosis, science focuses on three major communication routes:
- Neural pathway — The vagus nerve acts as a two‑way highway between gut bacteria and the brain.
- Endocrine pathway — Microbes influence hormones and neurotransmitters that regulate stress, including cortisol.
- Immune pathway — Disbiosis triggers systemic inflammation, which can cross the blood–brain barrier and activate depressive or anxious responses.
Links Between Psychodysbiosis and Mental Disorders
Research has found associations between psychodysbiosis and several conditions:
- Depression — reduced bacterial diversity and elevated inflammatory markers
- Anxiety — increased intestinal permeability (“leaky gut”)
- Autism (ASD) — presence of specific bacteria affecting sensory processing
- ADHD — imbalances in microbial production of dopamine precursors
While causality is still being studied, the correlations are strong and consistent.
Psychobiotics: The Therapeutic Counterpart
As a response to psychodysbiosis, psychobiotics have emerged — specific probiotic strains such as Lactobacillus helveticus or Bifidobacterium longum that show measurable benefits in mental health.
How Burnout Triggers Psychodysbiosis
Burnout places the body in a state of chronic alertness, activating the HPA axis and flooding the system with cortisol. This cascade leads to:
- Hyper‑cortisolemia — excess cortisol increases intestinal permeability (“leaky gut”)
- Reduced mucosal protection — stress decreases mucin production, weakening the intestinal barrier
- Low‑grade inflammation — bacterial fragments enter the bloodstream, triggering immune responses that affect the brain
This is why burnout is not just psychological — it becomes physiological.
Symptoms of Psychodysbiosis Caused by Burnout
People experiencing burnout often show clear signs of psychodysbiosis:
- Brain fog — difficulty concentrating or making simple decisions
- Selective cravings — pathogenic bacteria “demand” sugar and processed foods
- Visceral irritability — mood swings that feel like they originate in the gut
- Non‑restorative fatigue — waking up tired due to impaired neurotransmitter production
The Vicious Cycle: Burnout ↔ Psychodysbiosis
The most dangerous aspect is the self‑reinforcing loop:
- Work stress disrupts the microbiota → psychodysbiosis
- The altered microbiota stops producing serotonin and GABA
- Stress tolerance collapses
- Burnout deepens
This cycle continues unless both the mind and the gut are addressed.
Breaking the Cycle: What Science Suggests
Recovering from burnout requires more than rest or psychological therapy. Supporting gut health is essential. General strategies include:
- Anti‑inflammatory diet — reducing sugar and increasing fermentable fiber
- Psychobiotics — certain strains have been shown to reduce cortisol levels
- Vagus nerve regulation — breathing techniques that signal safety to the gut